Doctors immediately accused Nadja of having diabetes when her daughter was born with low blood sugar. A year of uncertainty, remorse, and sleepless nights ensued. It wasn’t until several months later that it was evident her daughter had a rare genetic form of hyperinsulinism. Nadja tells her real experience today in an effort to increase awareness and offer other impacted families hope.
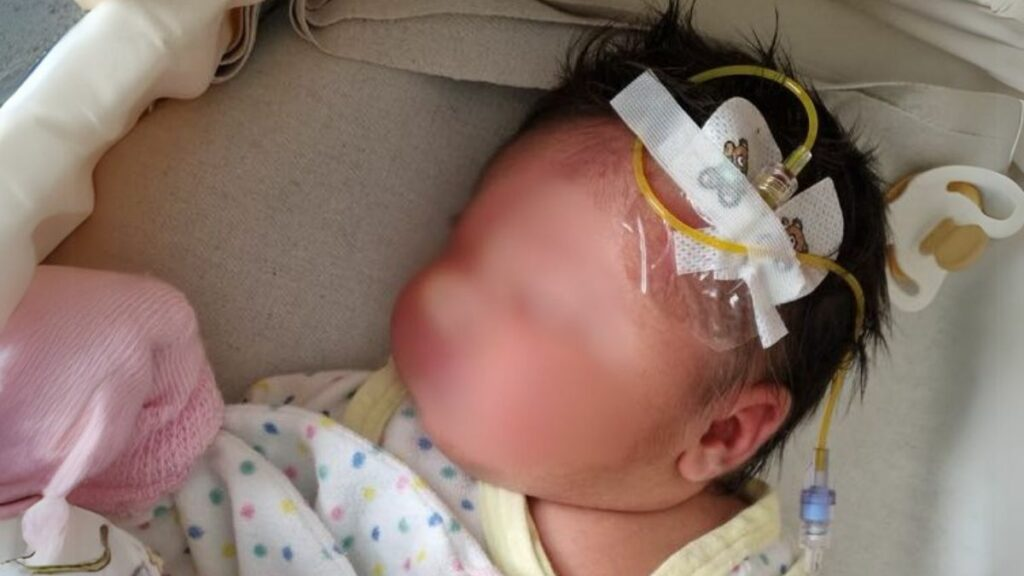
My daughter was born with neonatal hypoglycemia, or low blood sugar. If left undetected and untreated, these hypoglycemic episodes can lead to brain damage, developmental delays, epilepsy, or even d.e.a.t.h.
Short-term low blood sugar in infants can be caused by a number of factors, including stress, birth trauma, infections, and hormonal imbalances. It seems that my daughter’s type 1 diabetes was promptly determined to be the source of her condition. This resulted in a tearful journey,
A journey of despair and anger began.
And it wouldn’t finish until more than 400 kilometers from home, a year later. However, we were clueless. When blood sugar levels are poorly managed throughout pregnancy and are regularly and chronically elevated, women with diabetes are more likely to experience neonatal hypoglycemia.
I knew this, which is why I took exemplary care of my blood sugar management. When I became pregnant, I had already been an insulin-dependent diabetic for 20 years , had an insulin pump, and a glucose sensor. I wanted to avoid harm to my child, so I was very disciplined.
That’s why my blood sugar levels were close to those of a healthy person.
The neonatal doctors started our daughter on glucose infusions after her blood sugar still wasn’t rising 10 hours after birth, and they predicted that everything would be fine in 1-3 days . This is usually how long a baby’s body needs to adjust to its own insulin production.
But the third day came, and our daughter was still dependent on a high dose of glucose to maintain her blood sugar. And so the first week and then the second passed. Although her condition improved, we still had to feed her consistently every three hours and add extra dextrose to her bottle.
This was the only way she could achieve blood sugar levels that were still low but no longer life-threatening.
The doctors repeatedly questioned my blood sugar control and even debated the accuracy of my continuous monitoring sensor. It seemed as if there was only one possible explanation: that I was the one responsible for my daughter’s condition.
The mood kept getting worse during the third week in the NICU. With consistent three-hour breastfeeding, our young daughter was finally able to maintain her blood sugar levels just over 60 mg/dl. The physicians decided that was sufficient, and I started to get the impression that they were gradually attempting to remove us.
I also wanted to go home, but felt incredibly unsafe.
I later learned that this was justified. According to guidelines and expert opinion, infants with such prolonged hypoglycemia should not be discharged until they can maintain a stable blood sugar level above 70 mg/dl after six hours of fasting.
After 21 days, we were discharged with a diagnosis of transient (temporary) neonatal hyperinsulinism. However, we were told to continue breastfeeding every three hours . We didn’t have to monitor our blood sugar at home, as it would be stable. We weren’t told when we could try longer periods without breastfeeding, especially at night.
We should be happy!
Other families would have to feed every two hours after being released from the hospital. Since our daughter only experienced adjustment issues due to my (ostensibly poorly managed) diabetes, she would quickly “grow out of it.” However, in order to maintain stable blood sugar levels, I continued to nurse her every three to four hours as the months went by.
In reality, however, our mouse’s need to breastfeed was much lower and so she had to be actively woken up to breastfeed , especially at night, in order to get her to drink actively, with a lot of patience and tears.
I had the feeling that none of this was normal.
So I took her to a metabolic outpatient clinic. By now, I suspected that her condition might be due to a genetic defect. Hyperinsulinism can be triggered by a number of different defective genes.
Two of these trigger hyperinsulinism in combination with Mody diabetes. This is a very specific form of diabetes. Because it’s a genetic defect, this condition is passed down through multiple generations. Both my mother and my brother have diabetes, so it made sense!
But here too I was not taken seriously.
A genetic defect would be highly unlikely, but if I wanted to investigate it, I would have to get tested. Three months later, my blood work confirmed that I don’t have type 1 diabetes in the clinical sense , and the genetic test showed a defect in HNF4a.
Three months later, my daughter received the same result. She was 9 months old by then. Besides HNF4a, there are eight other genes associated with hyperinsulinism , but it is suspected that there are other defective genes that
trigger this disease.
I was still breastfeeding every 2-4 hours (day and night) to somehow keep our daughter’s blood sugar stable.
I, my family, and my breastfeeding relationship with my kid were all under tremendous stress as a result of the entire circumstance. For both of us, breastfeeding became mandatory.
I was simply overstimulated, overwhelmed, and desperate. Since we understood that this couldn’t continue indefinitely, we got in touch with the University Hospital of Düsseldorf. Our young girl was admitted to our hospital the week following her first birthday by a specialist in hyperinsulinism, which we learned about after doing a lot of research.
In the clinic, she had to fast for 14 hours overnight and her blood sugar was closely monitored.
It broke my heart, but afterward, we knew for sure that her body was still secreting too much insulin. A year after we were told she would soon outgrow her condition . A year after we were told we shouldn’t/didn’t need to monitor her blood sugar anymore.

Fortunately, the likelihood of severe hypoglycemia was now considered very low, but to ensure a normal daily routine in which she could eat whenever and however much she wanted, we would have to give her medication, which we did.
Since then, not only has a huge burden been lifted from us, but a bit of normality has finally returned.
At last, our daughter is free to sleep for as long as she desires at night. We can finally consider starting childcare now that I don’t freak out when she throws food around during the day.
Even today, I’m incredibly angry when I think that we could have been spared all the stress that first year if the neonatal doctors hadn’t been so biased ! If I had followed their advice and just left things as they were, my daughter would probably have suffered severe hypoglycemia several more times and perhaps suffered long-term damage.
But unfortunately this is not uncommon.
We’ve found a global online community of parents of affected children. We often hear that children are diagnosed with hyperinsulinism months later, after severe hypoglycemia.
This is often because blood glucose testing in infants is not standard procedure and there is little education about the disease . Additionally, parents are often unaware that they may have passed on a defective gene to their children.
I’m processing my time in the neonatal unit through therapy and can only hope for my daughter that she won’t remember that difficult first year later.”